Connections & integrations
Company news
Loading...
Loading...
September 2020
API
More flexibility for new hire enrollments
API
Support for accident and critical illness plans
August 2020
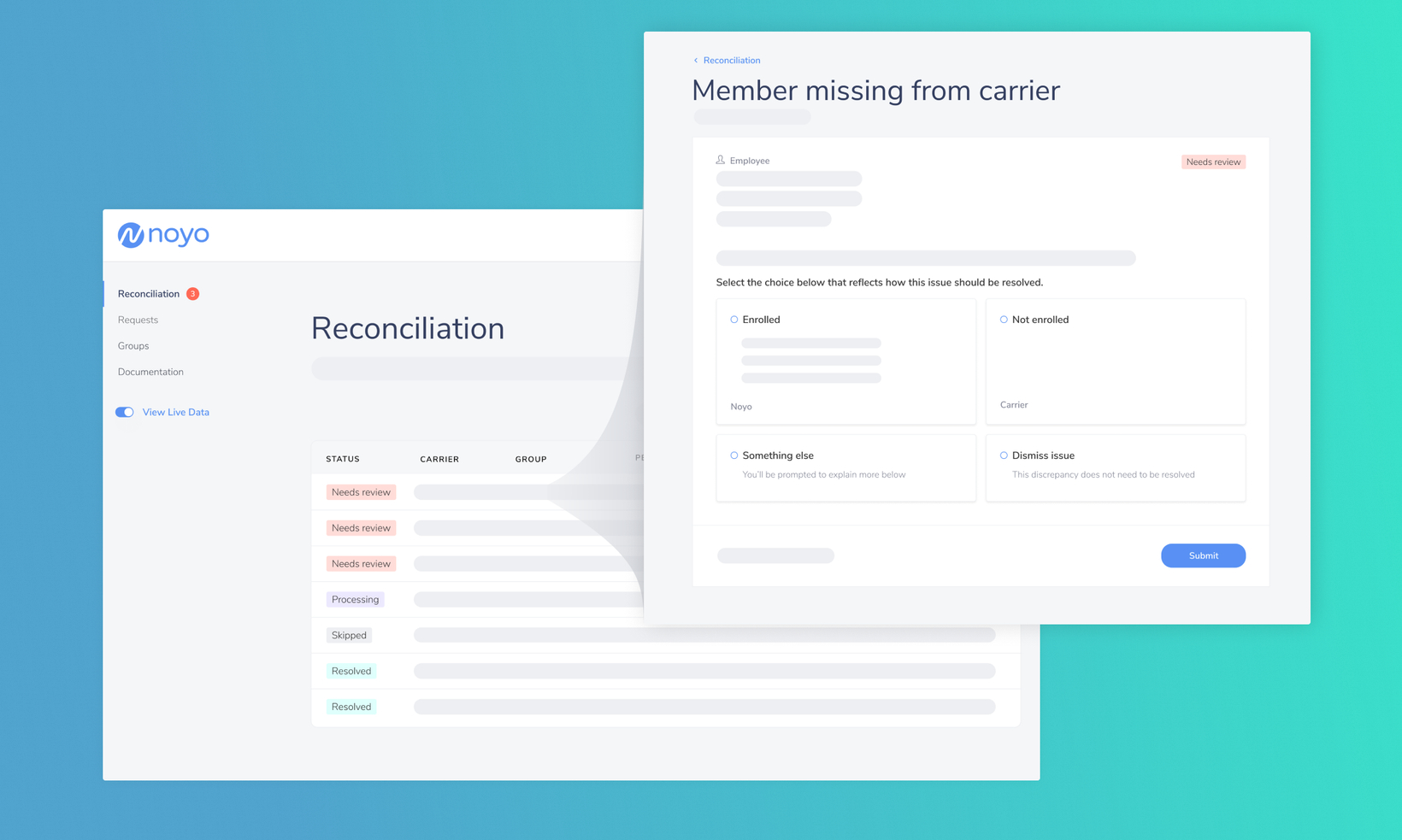
Command Center
Reconciliation: A powerful new tool for benefits administration platforms
API
Map groups and find records faster
API
Connections & integrations